International Volunteers in Urology Trip to Kigali, Rwanda
Jeremy Myers 3/17/2014 – University of Utah and International Volunteers in Urology****
I am just returning from a 2 week trip from Rwanda, Africa with the International Volunteers in Urology (IVUmed). The focus of this group, headed, by Catherine DeVries MD, is on increasing global urologic access through education of local surgeons. The motto of the organization is “teach one reach many.” This philosophy differs substantially from many relief organizations or mission trips. Most often these trips seek to give aid and provide surgical care in resource-poor countries. While this is a noble sentiment, the impact of these trips may not be very great when they are viewed in the context of a country’s overall population and needs. How much impact can a single trip have, with 20-40 operations performed in a country with a population of millions? This is why IVUmed’s mission and guiding principles are so important. As opposed to impacting a few patients, surgeons can impact a population by identifying sites where surgeons are wanting to increase the level of care they provide and have the basic resources needed to create this change.
In Rwanda, there are 2 urologists for a population of 12 million people! They are talented surgeons that are concentrated on providing quality care and also upon training more urologists. They are now training 2 other urologists and anticipate a residency in urology in the future.
Our trip was the first adult reconstructive urology workshop in Rwanda. We found that the surgeons there were very talented. They had excellent fine dissection and made the most of the resources they had. They perform about 50-60 urethroplasties a year and were quite expert at buccal grafting. The Rwandan surgeons, however, did not perform perineal urethroplasty for pelvic fracture, and instead, would do transpubic urethroplasty. We were able to demonstrate the perineal approach in 6 patients with pelvic fracture urethral injury. They were impressed with this more refined approach and should be able to incorporate it into their skill set with their already impressive urethroplasty experience. In addition, we performed 2 augmentation cystoplasties with the creation of catheterizable channels in patients with spinal cord injury and obstructing urethral strictures. These were challenging cases, but not something the Rwandan surgeons had had much exposure to.
Our team consisted of 2 adult reconstructive urologists, a urology resident, a radiologist who was married to one of the reconstructive urologists, and an anesthesiologist. We performed about 26 operations in 2 weeks; 18 of these operations were urethroplasties.
We were able to have the weekend in Kigali, which is the main city in Rwanda. Our weekend was spent visiting the markets in the city and relaxing. We also made a visit to the genocide museum. While this was a difficult visit to make, we felt this was something important to do in order to understand how the genocide has affected all of Rwanda and shaped its current government and culture.
This was a fantastic trip and our team felt we were able to educate and show the Rwandan surgeons some advanced techniques that they can incorporate very readily into their practice. I am looking forward to returning and reinforcing these techniques and observing what progress the urologist have made in shaping their urology training programs. They were inspiring surgeons and individuals and very gracious hosts for our trip. While it takes a while to get to Rwanda, the experience was worth it.
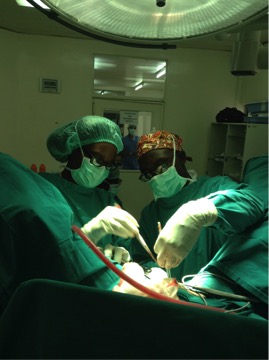
Fenwa Famakinwa, (resident from University of Chicago) assisting in urethroplasty with Dr. Eduoard Ngendahayo, the current urology fellow at the King Faisel Hospital, Kigali, Rwanda, March 2014.
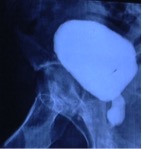
A retrograde urethrogram and voiding cystourethrogram in a patient with a posterior urethral injury from a gunshot wound to the pelvis.
